Person-centred care for musculoskeletal pain — a tool to put principles into practice
Lauren Finestone
Person-centred care is an important part of care for people with musculoskeletal pain conditions. But evidence that some healthcare professionals struggle to integrate person-centred care principles into their clinical practice. A tool that provides a structured approach can help.Person-centred care involves seeing the patient as a whole person. It means taking a biopsychosocial perspective to understanding and managing their condition, involving them in the treatment process and fostering a strong therapeutic alliance.
It’s about recognising that patients’ medical needs are best understood and addressed in the context of their entire lives — including ‘their life goals and social, economic, emotional and spiritual functioning’.
But this can be challenging to do in practice. Limited time and resources, lack of knowledge and skills and a lack of tools can be obstacles to clinicians applying person-centred principles in different clinical scenarios.
This article summarises a practical framework that can help clinicians put the principles of person-centred care into practice in their management of people with musculoskeletal pain conditions.
The framework has 4 principles and 3 phases. Let’s start with the 3 phases:
1. Identification and goal setting (and shared decision-making)
This is where the clinician:
- identifies the patient’s experiences, ideas and beliefs about their pain experience
- evaluates their attitude, self-efficacy, social influence and self-management skills
- evaluates their expectations, openness toward self-management and readiness to change.
This Self-management identification tool can support clinicians to evaluate self-management topics:
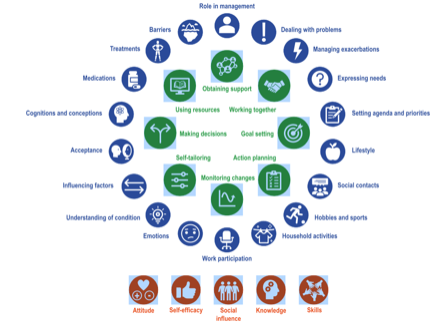
Once this has been done, the clinician and patient can set goals that are based on the patient’s values, preferences and needs. Value-based goal setting promotes open communication about motivations and can reveal the things that are likely to support and get in the way of self-management.
Shared decision-making is an important aspect of self-management support. This is when clinicians and patients work together to make decisions and set goals that are based on the available evidence and the patient’s individual preferences, beliefs, and values.
It ensures the patient understands the risks, benefits and possible consequences of different options and is empowered to make decisions about the care that is right for them (including choosing no treatment).
It may also increase patients’ satisfaction, engagement, adherence and ability to self-manage their symptoms.
2. Coaching to self-management
Clinicians should use a self-management approach that tailors treatment for people with musculoskeletal pain conditions.
How much focus there is on self-management will depend on the patient’s characteristics, needs and goals and the duration of their signs and symptoms.
Self-management is informed by evidence-based treatments and recommendations for managing musculoskeletal pain conditions.
Publications about self-management support for people with musculoskeletal conditions are valuable resources for clinicians.
Although the self-management approach originates from the treatment of chronic or persistent conditions, it can be used more generally in physiotherapy for people with musculoskeletal pain conditions — including acute conditions.
The goal is to empower patients to take an active role in managing their condition and to function as best they can. It’s important that physiotherapists have the knowledge, skills and confidence to support this approach.
General self-management skills
The ultimate aim of self-management support is to improve a patient’s quality of life by encouraging them to obtain the skills they need to actively manage their condition in the short- and long-term. General self-management skills can support this aim. But they are often overlooked by clinicians.
General self-management skills are things like problem solving, decision-making, using resources, forming a patient-provider partnership, action planning, self-tailoring, and self-monitoring.
Improving these skills could be a goal for people who were found to lack general self-management skills in the identification and goal setting phase.
Specific knowledge, skills and tools
Specific skills, knowledge and tools can then be added, based on the patient’s context, experience and presentation. These topics could include :
- dealing with and accepting pain, disability, exacerbations, emotions, fatigue and stress
- physical barriers to recovery (like a graduated exercise program of adequate dosage)
- lifestyle factors (physical activity, sleep, weight control, nutrition and relaxation)
- unhelpful thoughts and beliefs
- strategies to support work and social participation
Since behaviour change can be an important part of self- management, it’s valuable to include factors that determine behaviour —attitude, self-efficacy, social influence in the support provided, not just providing educational information about these topics or skills.
It’s also important to pay attention to potential barriers to self- management. Since self-efficacy is one way to achieve self-management, setting patients up for successful experiences is important.
3. Evaluation and follow-up
Reassessment and reflection are essential parts of any treatment, including supported self-management.
It’s also important to help people plan for the future. That also involves making an action plan to deal with future challenges and relapses.
This could also include a follow-up plan, which could consist of online or phone consults, email contact or an in-person review appointment after several months.
Objective measurements (like questionnaires) should be used to evaluate the patient’s understanding of their condition, self-management skills and perceived self-efficacy.
The principles that underly the phases
The therapeutic relationship
The therapeutic relationship underpins the whole the framework. This is the safe, collaborative professional and personal relationship the patient and physiotherapist develop.
Research shows that better quality relationships between clinicians and patients can lead to improved clinical outcomes, satisfaction with services and adherence to treatment plans in people with musculoskeletal conditions.
To establish this relationship, healthcare professionals should show empathy and be present, receptive, committed and genuine with their patients.
It can be challenging to move from intention to action without a structured approach. The framework can helps clinicians identify what to do in the moment and to reflect on what to do in future interactions.
A biopsychosocial understanding of the patient's pain experience
Healthcare professionals often struggle to address the psychosocial aspects of a patient's condition and tend to focus on the biomedical and biomechanical aspects instead.
But person-centred care should consider all the factors that contribute to a person's pain experience. This includes the biopsychosocial consequences of the condition for the individual and the support they need to overcome challenges and barriers to managing their condition.
Person-focused communication
Person-centred care involves using a collaborative communication style that includes the patient's perspective into the therapeutic process.
This requires communicating with the person throughout the clinical interaction in a validating, considerate and non-judgmental way. It means paying attention to both what is said and how it is said, and to both verbal and nonverbal language.
This allows healthcare professionals to better understand their patients' needs and goals, and to co-design a personalised management plan to get the patient back to doing what’s important to them.
Supported self-management
Clinicians should support people with musculoskeletal conditions do develop the skills that allow them to actively participate in and take responsibility for managing their condition — even after the initial treatment period has ended — so they can function at their best.
Original research
Hutting, N., Caneiro, J. P., Ong'wen, O. M., Miciak, M., & Roberts, L. (2022). Person-centred care for musculoskeletal pain: Putting principles into practice. Musculoskeletal Science and Practice, 102663.

