Mapping Australian systems of income support

Australia has ten major systems of income support for Australian workers unable to do their job because of injury or illness – from sick leave to workers compensation to private insurers to Centrelink payments.
A new report suggests that missed opportunities in one scheme, for example, workplace injury management programs, may be placing pressure on other schemes.
This is something I, in my work as an Occupational Physician, have seen many times. Consider the following case study, a composite of real life situations I’ve encountered.
Catherine is a 46-year-old bank teller involved in a motor vehicle accident. She sustained whiplash and a fracture of one of the small bones in her right wrist. Over the two years prior to the accident she’d had a poor relationship with her manager. After the accident she was off work for a few months and during that time started consuming more alcohol.
By the time she resumed work her alcohol consumption was affecting her to the extent she was coming to work late and missing days of work. Her manager became frustrated and began pressuring Catherine to attend work regularly and on time.
Feeling unsupported and under pressure, Catherine lodged a compensation claim for bullying which was subsequently accepted. She reported ongoing neck and hand pain and said that these problems meant she couldn’t do her job. She was diagnosed with an adjustment disorder, a psychological condition that can occur when someone has trouble coping with a stressful life event.
Catherine ceased work after a few months and didn’t get back to her job. There were cursory attempts at helping her find another job, but in the end she stayed on the compensation system for two and a half years, receiving payments.
Catherine then lodged a claim for incapacity payments through her superannuation fund. She continued on those payments for another two years. There was dispute about whether she could return to work after that period, or whether she was totally and permanently disabled for work. She engaged solicitors and after 20 months her claim for total and permeant disability was accepted, with a lump sum payment of $420k.
After a non-entitlement period because of the lump sum payment, Catherine transitioned to Centrelink payments.
Difficult workplace relationships, a failure of the workers’ compensation system to promote rehabilitation, and personal circumstances all fed into Catherine’s failure to return to work: and she, her insurer and the government each paid a high cost.
Let’s take a look at the current situation, as described by the Insurance Work and Health Group at Monash University published The Cross Sector Project: Mapping Australian Systems of Income Support for People with Health Related Work Incapacity.
Overview of income support in Australia
The cost of income support for Australians with work incapacity in just one year (2015/16) was $37.2 billion. These costs were covered by a complex array public and private entities, which can be broadly grouped as:
- Employers, who spent $18.7 billion supporting 6.5 million workers with short-term work incapacity (e.g. via sick leave);
- Social security systems, which spent $8.6 billion on 469,000 Australians with long term work incapacity (primarily via the disability support pension);
- Workers compensation schemes, which spent $2.5 billion on 156,000 claimants across Australia;
- Life insurance companies, which paid out $4.4 billion on 95,000 claimants (via total and permanent disability payments and income protection policies); and
- Motor vehicle accident compensation schemes, which provided statutory benefits to 6,000 Australians.
In theory, if not always practice, Australian systems of income support provision share the following four goals:
- Reducing the severity and duration of work incapacity where it occurs;
- Improving engagement in work; and
- Minimising the costs of work incapacity to society, workers and employers.
However, there is a great deal of variability between systems in terms of the services offered to Australians with work incapacity.
Who gets what?
For an individual worker, entitlement to services depends on which income support system they’re eligible to access.
Each of the systems offers some form of case management: this is the only service provided across the board, and the details of the support offered vary widely.
Other relevant services include:
- Return to work services (i.e. resumption of the same job, or a new role at the same workplace);
- Healthcare and treatment;
- Job finding or employment services; and
- Functional support services (i.e. aids and equipment to support daily living.
Workers compensation schemes offer some form of all these services to both short term and long term claimants. Employers tend to offer case management and RTW services, but none of the others. People injured in a motor vehicle accident may have access to all of these services if they opt for ongoing no-fault government-funded compensation, or just two of these services (case management and healthcare and treatment) if they sue for a one-off lump sum payment. The federal government social security system can offer support with job seeking and retraining.
System to system flow
People move between the systems, but we don’t currently have a lot of information about how this flow occurs.
For example, in most systems injured workers are eligible for workers’ compensation for a limited period of time. At that point, most people leave the workers’ compensation system and we don’t know what happens to them. How many go onto the disability system? How many get another job? How many make a claim through life insurance? We simply don’t know – which means we don’t really understand the economic and societal costs.
Together with experts they interviewed in the preparation of the report, the researchers identified seven likely patterns of movement between systems, described in the table below.
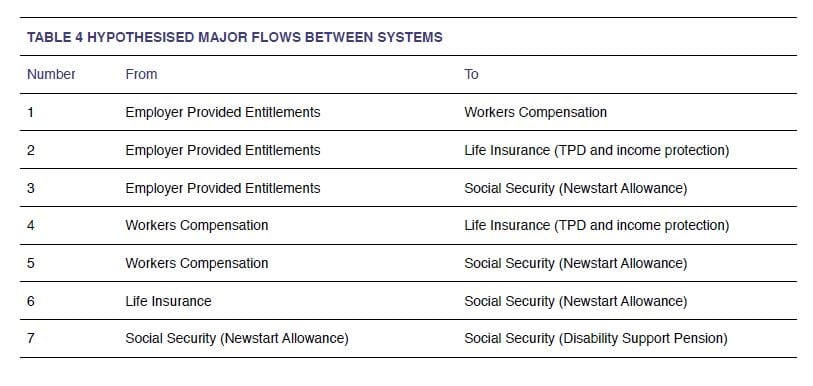
If these hypothesised flows are correct, workplace systems and workers’ compensation schemes are pivotal. The ways in which these schemes are managed may direct vulnerable workers towards recovery and productivity or entrenched disability and reliance on external financial support, including lump sum payments from insurers.
If rehabilitation efforts in upstream services (workers compensation, individual workplaces) are inadequate, downstream services (social security, life insurers) ultimately foot the bill.
How can we do better?
Firstly, we need to focus rehabilitation efforts on upstream systems: specifically workplace injury management systems, workers’ compensation systems and car accident systems.
Secondly, we need to create better connections between income support systems. There needs to be more data sharing and more consistency in terms of the data collected. At the moment we have informed hypotheses about how and why people move between systems: we need to look at what’s actually happening.
Thirdly, we need to look beyond our silos towards the bigger picture. We can’t afford to focus only on one system, particularly when thinking about cost-effectiveness.
This report begins this process.
Original research
Collie, A., Iles, R. and Di Donato M.F. The Cross Sector Project: Mapping Australian Systems of Income Support for People with Health Related Work Incapacity. Insurance Work and Health Group, Faculty of Medicine Nursing and Health Sciences, Monash University (2017).

