Why we are pro best practice case management

"The field of case management has long suffered from a lack of credible proof that it has an impact on claim costs because no-one has been willing to set up a study to test that hypothesis. Here’s a study that does just that!" - Jennifer Christian.
Dr Jennifer Christian, MD, MPH
President, Webility Corporation (www.webility.md)
Chair, 60 Summits Project (www.60summits.org)
Chair, American College of Occ. & Env. Medicines Work Fitness & Disability Section (www.acoem.org)
Moderator, Work Fitness & Disability (https://groups.io/g/WFDRoundtable)
Between 2000 and 2003, a return to work case management approach was implemented and studied across a series of medium to large-sized companies in Victoria. The organisation running the case management approach was called OccCorp – a privately run group set up to introduce and provide streamlined care and early return to work when an employee was injured.
The case management based intervention was based on approaches recognised as evidence-based practice;
- Connecting with the employee early,
- Streamlining return to work,
- Engagement of both the employee and line manager in the shaping of modified duties;
- Assisting the worker to get rapid access to good quality medical care, and
- Overcoming the multitude of obstacles that can get in the way of consistent return to work.
A more detailed account of the case management model is here. In this article, I describe the quantifiable benefits that came from this worker-centred approach.
As there is a centralised database of all compensation claims in Victoria, it is possible to gather all relevant claims information.
WorkSafe, then known as WorkCover, provided claims information for the companies where the case management approach was put in place.
Claims data that covered the same time period before the model was put in place was also provided for those companies. The claim results before and during the years of the case management (intervention) approach were then compared.
Claims information for control companies was also provided by WorkSafe. Control companies were similar organisations where the case management approach was not put in place. They were randomly selected from the WorkSafe database by WorkSafe, after being matched for industry type and company size.
Including a control group is important as there could be external factors that influence the return to work results. For example, if there was a change in the legislation such as a drop in the wages paid through WorkCover, return to work may change across the state. Having a control group allows the same comparisons to be done in the control group to check if outside factors influenced the results.
The figure below shows the four groups studied.
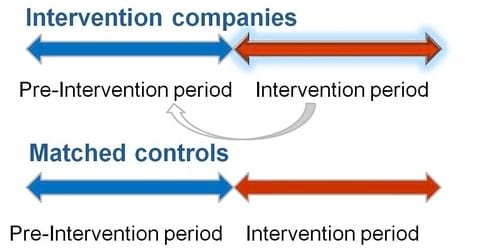
There were approximately 800 claims in the case management companies across the time periods before and during the case management approach. There were three control claims for each claim in the case management companies. The larger the number of claims in the study makes the study more reliable (see sample size http://en.wikipedia.org/wiki/Sample_size_determination).
The study used claim information from WorkSafe. The main information assessed was:
- Days lost from work;
- Average claim costs;
- Costs of medical care.
Study results
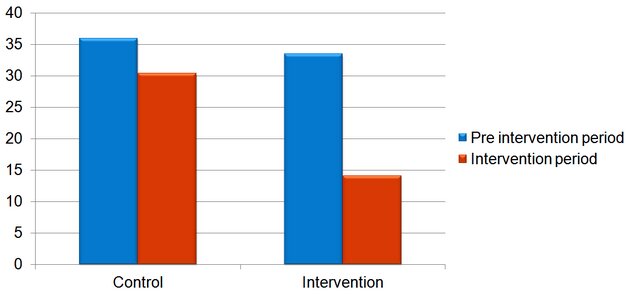
The graph below shows the average days lost from work in claims across the case management and control companies, before the intervention was put in place and during the intervention period.
In the companies where the case management model was introduced the average days lost from work per claim dropped by 58% (from 34 days to 14 days). There was also a drop in the days lost from work in the control group, but this was smaller. The drop was highly statistically significant in the case management group but not in the control group.
Days lost from work in case management intervention and control companies, before and during the intervention period
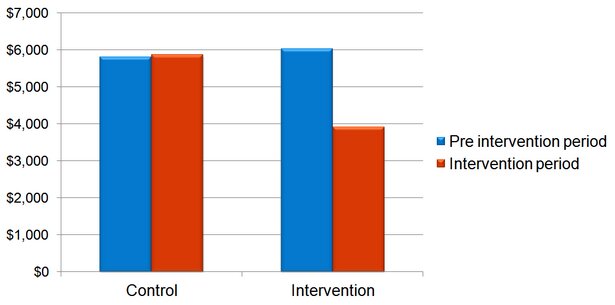
Average claim costs paid during the respective periods are shown below.
In the case management companies claims cost dropped by 35%, from approximately $6,000 to $4,000. There was no such change in the control companies
Average claims costs in case management intervention and control companies, before and during the intervention period
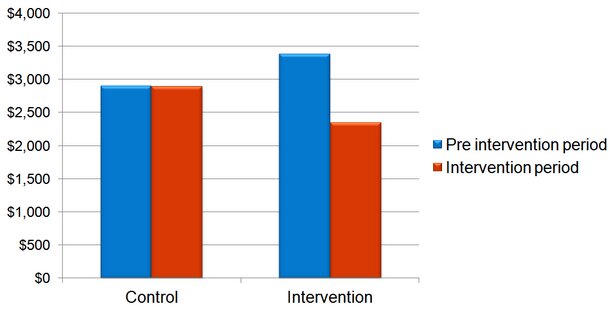
The average medical costs are shown below. The medical costs were higher in the intervention companies before the case management approach was put in place. Medical costs were reduced by 31% in the companies where the intervention was introduced.
Average medical costs in case management intervention and control companies, before and during the intervention period
The reduction in days lost from work occurred across industry types, company size as measured by payroll, and the body part affected.
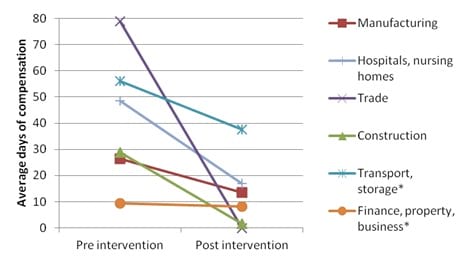
Average days of compensation before and during case management intervention periods, by industry type
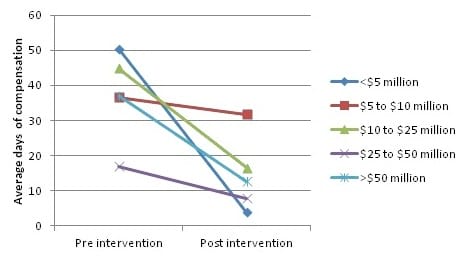
Average days of compensation before and during intervention periods, by company size as measured by payroll
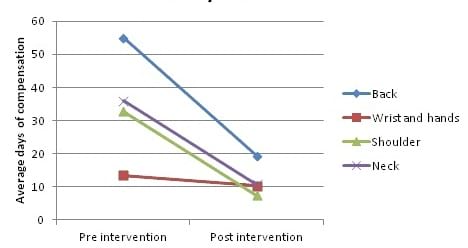
Average days of compensation before and during intervention periods, by body injury location
Summary – Quality outcomes come from quality care
In Victoria we are fortunate to have a centralised system where all claims information is collected and stored. This allowed comparison of the results of a case management approach that focused on early access to good medical care, cooperation at the workplace and return to work.
This case management approach was based on supporting the employee and enhancing cooperation. You can read a fuller description of the model here.
The results show the elements of return to work we have all been discussing for the last two decades can be effective when put together in a streamlined approach. The case management results show better return to work outcomes can be achieved. They show that the spotlight should be aimed at developing cooperation at the workplace, early help for the employee, and engaging line managers and senior managers.
Published 01 November, 2012 | Updated 19 October, 2021

